Abstract
As antiretroviral therapy (ART) becomes increasingly affordable and accessible to women of childbearing age across the globe, the number of children who are exposed to Human Immunodeficiency Viruses (HIV) but remain uninfected is on the rise, almost all of whom were also exposed to ART perinatally. Although ART has successfully aided in the decline of mother-to-child-transmission of HIV, the long-term effects of in utero exposure to ART on fetal and postnatal neurodevelopment remain unclear. Evaluating the safety and efficacy of therapeutic drugs for pregnant women is a challenge due to the historic limitations on their inclusion in clinical trials and the dynamic physiological states during pregnancy that can alter the pharmacokinetics of drug metabolism and fetal drug exposure. Thus, much of our data on the potential consequences of ART drugs on the developing nervous system comes from preclinical animal models and clinical observational studies. In this review, we will discuss the current state of knowledge and existing approaches to investigate whether ART affects fetal brain development, and describe novel human stem cell-based strategies that may provide additional information to better predict the impact of specific drugs on the human central nervous system.

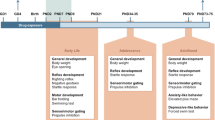
Approaches to evaluate the impact of drugs on the developing brain. Dysregulation of the developing nervous system can lead to long-lasting changes. Integration of data from animal models, clinical observations, and cell culture studies is needed to predict the safety of therapeutic antiretroviral drugs during pregnancy. New approaches include human induced pluripotent stem cell (iPSC)-based 2D and 3D models of neuronal networks and brain regions, as well as single cell profiling in response to drug exposure.



Similar content being viewed by others
References
Akay C, Cooper M, Odeleye A, Jensen BK, White MG, Vassoler F et al (2014) Antiretroviral drugs induce oxidative stress and neuronal damage in the central nervous system. J Neurovirol 20(1):39–53. https://doi.org/10.1007/s13365-013-0227-1
Alimenti A, Forbes JC, Oberlander TF, Money DM, Grunau RE, Papsdorf MP et al (2006) A prospective controlled study of neurodevelopment in HIV-uninfected children exposed to combination antiretroviral drugs in pregnancy. Pediatrics 118(4):e1139–e1145. https://doi.org/10.1542/peds.2006-0525
Allavena C, Le Moal G, Michau C, Chiffoleau A, Raffi F (2006) Neuropsychiatric adverse events after switching from an antiretroviral regimen containing efavirenz without tenofovir to an efavirenz regimen containing tenofovir: a report of nine cases. Antivir Ther 11(2):263–265
Apostolova N, Funes HA, Blas-Garcia A, Alegre F, Polo M, Esplugues JV (2015) Involvement of nitric oxide in the mitochondrial action of efavirenz: a differential effect on neurons and glial cells. J Infect Dis 211(12):1953–1958. https://doi.org/10.1093/infdis/jiu825
Arts EJ, Hazuda DJ (2012) HIV-1 antiretroviral drug therapy. Cold Spring Harb Perspect Med 2(4):a007161. https://doi.org/10.1101/cshperspect.a007161
Bale TL (2015) Epigenetic and transgenerational reprogramming of brain development. Nat Rev Neurosci 16(6):332–344. https://doi.org/10.1038/nrn3818
Barre-Sinoussi F, Chermann JC, Rey F, Nugeyre MT, Chamaret S, Gruest J et al (1983) Isolation of a T-lymphotropic retrovirus from a patient at risk for acquired immune deficiency syndrome (AIDS). Science 220(4599):868–871
Becquet R, Bland R, Leroy V, Rollins NC, Ekouevi DK, Coutsoudis A et al (2009) Duration, pattern of breastfeeding and postnatal transmission of HIV: pooled analysis of individual data from West and South African cohorts. PLoS One 4(10):e7397. https://doi.org/10.1371/journal.pone.0007397
Blanche S, Tardieu M, Rustin P, Slama A, Barret B, Firtion G et al (1999) Persistent mitochondrial dysfunction and perinatal exposure to antiretroviral nucleoside analogues. Lancet 354(9184):1084–1089. https://doi.org/10.1016/S0140-6736(99)07219-0
Boyd SD, Sampson MR, Viswanathan P, Struble KA, Arya V, Sherwat AI (2019) Cobicistat-containing antiretroviral regimens are not recommended during pregnancy: viewpoint. AIDS 33(6):1089–1093. https://doi.org/10.1097/QAD.0000000000002163
Brown LA, Jin J, Ferrell D, Sadic E, Obregon D, Smith AJ et al (2014) Efavirenz promotes beta-secretase expression and increased Abeta1-40,42 via oxidative stress and reduced microglial phagocytosis: implications for HIV associated neurocognitive disorders (HAND). PLoS One 9(4):e95500. https://doi.org/10.1371/journal.pone.0095500
Calamandrei G, Valanzano A, Puopolo M, Aloe L (2002) Developmental exposure to the antiretroviral drug zidovudine increases brain levels of brain-derived neurotrophic factor in mice. Neurosci Lett 333(2):111–114
Caniglia EC, Cain LE, Justice A, Tate J, Logan R, Sabin C et al (2014) Antiretroviral penetration into the CNS and incidence of AIDS-defining neurologic conditions. Neurology 83(2):134–141. https://doi.org/10.1212/WNL.0000000000000564
Caniglia EC, Phillips A, Porter K, Sabin CA, Winston A, Logan R et al (2018) Commonly Prescribed Antiretroviral Therapy Regimens and Incidence of AIDS-Defining Neurological Conditions. J Acquir Immune Defic Syndr 77(1):102–109. https://doi.org/10.1097/QAI.0000000000001562
Carvalhal A, Gill MJ, Letendre SL, Rachlis A, Bekele T, Raboud J et al (2016) Central nervous system penetration effectiveness of antiretroviral drugs and neuropsychological impairment in the Ontario HIV Treatment Network Cohort Study. J Neurovirol 22(3):349–357. https://doi.org/10.1007/s13365-015-0404-5
Chambers SM, Mica Y, Lee G, Studer L, Tomishima MJ (2016) Dual-SMAD Inhibition/WNT Activation-Based Methods to Induce Neural Crest and Derivatives from Human Pluripotent Stem Cells. Methods Mol Biol 1307:329–343. https://doi.org/10.1007/7651_2013_59
Chen Y, Balasubramaniyan V, Peng J, Hurlock EC, Tallquist M, Li J, Lu QR (2007) Isolation and culture of rat and mouse oligodendrocyte precursor cells. Nat Protoc 2(5):1044–1051. https://doi.org/10.1038/nprot.2007.149
Ciavatta VT, Bichler EK, Speigel IA, Elder CC, Teng SL, Tyor WR, Garcia PS (2017) In vitro and Ex vivo Neurotoxic Effects of Efavirenz are Greater than Those of Other Common Antiretrovirals. Neurochem Res 42(11):3220–3232. https://doi.org/10.1007/s11064-017-2358-x
Ciccarelli N, Fabbiani M, Di Giambenedetto S, Fanti I, Baldonero E, Bracciale L et al (2011) Efavirenz associated with cognitive disorders in otherwise asymptomatic HIV-infected patients. Neurology 76(16):1403–1409. https://doi.org/10.1212/WNL.0b013e31821670fb
Connor, E. M., Sperling, R. S., Gelber, R., Kiselev, P., Scott, G., O'Sullivan, M. J., . . . et al. (1994). Reduction of maternal-infant transmission of human immunodeficiency virus type 1 with zidovudine treatment. Pediatric AIDS Clinical Trials Group Protocol 076 Study Group. N Engl J Med, 331(18), 1173-1180. doi:https://doi.org/10.1056/NEJM199411033311801
Culnane M, Fowler M, Lee SS, McSherry G, Brady M, O'Donnell K et al (1999) Lack of long-term effects of in utero exposure to zidovudine among uninfected children born to HIV-infected women. Pediatric AIDS Clinical Trials Group Protocol 219/076 Teams. JAMA 281(2):151–157
De Schacht C, Mabunda N, Ferreira OC, Ismael N, Calu N, Santos I et al (2014) High HIV incidence in the postpartum period sustains vertical transmission in settings with generalized epidemics: a cohort study in Southern Mozambique. J Int AIDS Soc 17:18808. https://doi.org/10.7448/IAS.17.1.18808
Decloedt EH, Rosenkranz B, Maartens G, Joska J (2015) Central nervous system penetration of antiretroviral drugs: pharmacokinetic, pharmacodynamic and pharmacogenomic considerations. Clin Pharmacokinet 54(6):581–598. https://doi.org/10.1007/s40262-015-0257-3
Demir M, Laywell ED (2015) Neurotoxic effects of AZT on developing and adult neurogenesis. Front Neurosci 9:93. https://doi.org/10.3389/fnins.2015.00093
Di Lullo E, Kriegstein AR (2017) The use of brain organoids to investigate neural development and disease. Nat Rev Neurosci 18(10):573–584. https://doi.org/10.1038/nrn.2017.107
Dolmetsch R, Geschwind DH (2011) The human brain in a dish: the promise of iPSC-derived neurons. Cell 145(6):831–834. https://doi.org/10.1016/j.cell.2011.05.034
Eiden C, Peyriere H, Peytavin G, Reynes J (2011) Severe insomnia related to high concentrations of raltegravir. AIDS 25(5):725–727. https://doi.org/10.1097/QAD.0b013e32834465c8
Engle SJ, Blaha L, Kleiman RJ (2018) Best Practices for Translational Disease Modeling Using Human iPSC-Derived Neurons. Neuron 100(4):783–797. https://doi.org/10.1016/j.neuron.2018.10.033
Etherton MR, Lyons JL, Ard KL (2015) HIV-associated Neurocognitive Disorders and Antiretroviral Therapy: Current Concepts and Controversies. Curr Infect Dis Rep 17(6):485. https://doi.org/10.1007/s11908-015-0485-6
Fischl, M. A., Richman, D. D., Grieco, M. H., Gottlieb, M. S., Volberding, P. A., Laskin, O. L., . . . et al. (1987). The efficacy of azidothymidine (AZT) in the treatment of patients with AIDS and AIDS-related complex. A double-blind, placebo-controlled trial. N Engl J Med, 317(4), 185-191. doi:https://doi.org/10.1056/NEJM198707233170401
Ford N, Mofenson L, Shubber Z, Calmy A, Andrieux-Meyer I, Vitoria M et al (2014) Safety of efavirenz in the first trimester of pregnancy: an updated systematic review and meta-analysis. AIDS 28(Suppl 2):S123–S131. https://doi.org/10.1097/QAD.0000000000000231
Fowler MG, Flynn P, Aizire J (2018) What is new in perinatal HIV prevention? Curr Opin Pediatr 30(1):144–151. https://doi.org/10.1097/MOP.0000000000000579
Fowler MG, Qin M, Fiscus SA, Currier JS, Flynn PM, Chipato T et al (2016) Benefits and Risks of Antiretroviral Therapy for Perinatal HIV Prevention. N Engl J Med 375(18):1726–1737. https://doi.org/10.1056/NEJMoa1511691
Funes HA, Apostolova N, Alegre F, Blas-Garcia A, Alvarez A, Marti-Cabrera M, Esplugues JV (2014) Neuronal bioenergetics and acute mitochondrial dysfunction: a clue to understanding the central nervous system side effects of efavirenz. J Infect Dis 210(9):1385–1395. https://doi.org/10.1093/infdis/jiu273
Garcia-Otero L, Lopez M, Gomez O, Gonce A, Bennasar M, Martinez JM et al (2016) Zidovudine treatment in HIV-infected pregnant women is associated with fetal cardiac remodelling. AIDS 30(9):1393–1401. https://doi.org/10.1097/QAD.0000000000001066
Gatch MB, Kozlenkov A, Huang RQ, Yang W, Nguyen JD, Gonzalez-Maeso J et al (2013) The HIV antiretroviral drug efavirenz has LSD-like properties. Neuropsychopharmacology 38(12):2373–2384. https://doi.org/10.1038/npp.2013.135
Gilbert EM, Darin KM, Scarsi KK, McLaughlin MM (2015) Antiretroviral Pharmacokinetics in Pregnant Women. Pharmacotherapy 35(9):838–855. https://doi.org/10.1002/phar.1626
Goodsell DS (2015) Illustrations of the HIV life cycle. Curr Top Microbiol Immunol 389:243–252. https://doi.org/10.1007/82_2015_437
Gordon J, Amini S, White MK (2013) General overview of neuronal cell culture. Methods Mol Biol 1078:1–8. https://doi.org/10.1007/978-1-62703-640-5_1
Gray J, Young B (2009) Acute onset insomnia associated with the initiation of raltegravir: a report of two cases and literature review. AIDS Patient Care STDS 23(9):689–690. https://doi.org/10.1089/apc.2009.0012
Greene ND, Copp AJ (2014) Neural tube defects. Annu Rev Neurosci 37:221–242. https://doi.org/10.1146/annurev-neuro-062012-170354
Griffin TZ, Kang W, Ma Y, Zhang M (2015) The HAND Database: a gateway to understanding the role of HIV in HIV-associated neurocognitive disorders. BMC Med Genomics 8:70. https://doi.org/10.1186/s12920-015-0143-8
Ha JC, Nosbisch C, Abkowitz JL, Conrad SH, Mottet NK, Ruppenthal GC et al (1998) Fetal, infant, and maternal toxicity of zidovudine (azidothymidine) administered throughout pregnancy in Macaca nemestrina. J Acquir Immune Defic Syndr Hum Retrovirol 18(1):27–38
Harris M, Larsen G, Montaner JS (2008) Exacerbation of depression associated with starting raltegravir: a report of four cases. AIDS 22(14):1890–1892. https://doi.org/10.1097/QAD.0b013e32830e0169
Heaton RK, Clifford DB, Franklin DR Jr, Woods SP, Ake C, Vaida F et al (2010) HIV-associated neurocognitive disorders persist in the era of potent antiretroviral therapy: CHARTER Study. Neurology 75(23):2087–2096. https://doi.org/10.1212/WNL.0b013e318200d727
Jahanshad N, Couture MC, Prasitsuebsai W, Nir TM, Aurpibul L, Thompson PM et al (2015) Brain Imaging and Neurodevelopment in HIV-uninfected Thai Children Born to HIV-infected Mothers. Pediatr Infect Dis J 34(9):e211–e216. https://doi.org/10.1097/INF.0000000000000774
Jankiewicz M, Holmes MJ, Taylor PA, Cotton MF, Laughton B, van der Kouwe AJW, Meintjes EM (2017) White Matter Abnormalities in Children with HIV Infection and Exposure. Front Neuroanat 11:88. https://doi.org/10.3389/fnana.2017.00088
Jensen BK, Monnerie H, Mannell MV, Gannon PJ, Espinoza CA, Erickson MA et al (2015) Altered Oligodendrocyte Maturation and Myelin Maintenance: The Role of Antiretrovirals in HIV-Associated Neurocognitive Disorders. J Neuropathol Exp Neurol 74(11):1093–1118. https://doi.org/10.1097/NEN.0000000000000255
Jin J, Grimmig B, Izzo J, Brown LAM, Hudson C, Smith AJ et al (2016) HIV Non-Nucleoside Reverse Transcriptase Inhibitor Efavirenz Reduces Neural Stem Cell Proliferation in Vitro and in Vivo. Cell Transplant 25(11):1967–1977. https://doi.org/10.3727/096368916X691457
Jones DL, Rodriguez VJ, Alcaide ML, Weiss SM, Peltzer K (2019) The Use of Efavirenz During Pregnancy is Associated with Suicidal Ideation in Postpartum Women in Rural South Africa. AIDS Behav 23(1):126–131. https://doi.org/10.1007/s10461-018-2213-3
Kilewo C, Karlsson K, Ngarina M, Massawe A, Lyamuya E, Swai A et al (2009) Prevention of mother-to-child transmission of HIV-1 through breastfeeding by treating mothers with triple antiretroviral therapy in Dar es Salaam, Tanzania: the Mitra Plus study. J Acquir Immune Defic Syndr 52(3):406–416. https://doi.org/10.1097/QAI.0b013e3181b323ff
Knapp KM, Brogly SB, Muenz DG, Spiegel HM, Conway DH, Scott GB et al (2012) Prevalence of congenital anomalies in infants with in utero exposure to antiretrovirals. Pediatr Infect Dis J 31(2):164–170. https://doi.org/10.1097/INF.0b013e318235c7aa
Kondo T, Imamura K, Funayama M, Tsukita K, Miyake M, Ohta A et al (2017) iPSC-Based Compound Screening and In Vitro Trials Identify a Synergistic Anti-amyloid beta Combination for Alzheimer's Disease. Cell Rep 21(8):2304–2312. https://doi.org/10.1016/j.celrep.2017.10.109
Lancaster MA, Renner M, Martin CA, Wenzel D, Bicknell LS, Hurles ME et al (2013) Cerebral organoids model human brain development and microcephaly. Nature 501(7467):373–379. https://doi.org/10.1038/nature12517
Lange SC, Bak LK, Waagepetersen HS, Schousboe A, Norenberg MD (2012) Primary cultures of astrocytes: their value in understanding astrocytes in health and disease. Neurochem Res 37(11):2569–2588. https://doi.org/10.1007/s11064-012-0868-0
Latronico T, Pati I, Ciavarella R, Fasano A, Mengoni F, Lichtner M et al (2018) In vitro effect of antiretroviral drugs on cultured primary astrocytes: analysis of neurotoxicity and matrix metalloproteinase inhibition. J Neurochem 144(3):271–284. https://doi.org/10.1111/jnc.14269
Lian, H., Roy, E., & Zheng, H. (2016). Protocol for Primary Microglial Culture Preparation. Bio Protoc, 6(21). doi:10.21769/BioProtoc.1989
Ma Q, Vaida F, Wong J, Sanders CA, Kao YT, Croteau D et al (2016) Long-term efavirenz use is associated with worse neurocognitive functioning in HIV-infected patients. J Neurovirol 22(2):170–178. https://doi.org/10.1007/s13365-015-0382-7
Marra CM, Zhao Y, Clifford DB, Letendre S, Evans S, Henry K et al (2009) Impact of combination antiretroviral therapy on cerebrospinal fluid HIV RNA and neurocognitive performance. AIDS 23(11):1359–1366. https://doi.org/10.1097/QAD.0b013e32832c4152
Marton RM, Miura Y, Sloan SA, Li Q, Revah O, Levy RJ et al (2019) Differentiation and maturation of oligodendrocytes in human three-dimensional neural cultures. Nat Neurosci 22(3):484–491. https://doi.org/10.1038/s41593-018-0316-9
McCormack SA, Best BM (2014) Protecting the fetus against HIV infection: a systematic review of placental transfer of antiretrovirals. Clin Pharmacokinet 53(11):989–1004. https://doi.org/10.1007/s40262-014-0185-7
McHenry MS, Balogun KA, McDonald BC, Vreeman RC, Whipple EC, Serghides L (2019) In utero exposure to HIV and/or antiretroviral therapy: a systematic review of preclinical and clinical evidence of cognitive outcomes. J Int AIDS Soc 22(4):e25275. https://doi.org/10.1002/jia2.25275
Mertens J, Marchetto MC, Bardy C, Gage FH (2016) Evaluating cell reprogramming, differentiation and conversion technologies in neuroscience. Nat Rev Neurosci 17(7):424–437. https://doi.org/10.1038/nrn.2016.46
Millet LJ, Gillette MU (2012) Over a century of neuron culture: from the hanging drop to microfluidic devices. Yale J Biol Med 85(4):501–521
Mitsuya H, Weinhold KJ, Furman PA, St Clair MH, Lehrman SN, Gallo RC et al (1985) 3'-Azido-3'-deoxythymidine (BW A509U): an antiviral agent that inhibits the infectivity and cytopathic effect of human T-lymphotropic virus type III/lymphadenopathy-associated virus in vitro. Proc Natl Acad Sci U S A 82(20):7096–7100
Montenegro-Burke JR, Woldstad CJ, Fang M, Bade AN, McMillan J, Edagwa B et al (2018) Nanoformulated Antiretroviral Therapy Attenuates Brain Metabolic Oxidative Stress. Mol Neurobiol. https://doi.org/10.1007/s12035-018-1273-8
Moren C, Noguera-Julian A, Rovira N, Garrabou G, Nicolas M, Cardellach F et al (2011) Mitochondrial assessment in asymptomatic HIV-infected paediatric patients on HAART. Antivir Ther 16(5):719–724. https://doi.org/10.3851/IMP1806
Nikolopoulou E, Galea GL, Rolo A, Greene ND, Copp AJ (2017) Neural tube closure: cellular, molecular and biomechanical mechanisms. Development 144(4):552–566. https://doi.org/10.1242/dev.145904
Noguera A, Fortuny C, Munoz-Almagro C, Sanchez E, Vilaseca MA, Artuch R et al (2004) Hyperlactatemia in human immunodeficiency virus-uninfected infants who are exposed to antiretrovirals. Pediatrics 114(5):e598–e603. https://doi.org/10.1542/peds.2004-0955
Nozyce ML, Huo Y, Williams PL, Kapetanovic S, Hazra R, Nichols S et al (2014) Safety of in utero and neonatal antiretroviral exposure: cognitive and academic outcomes in HIV-exposed, uninfected children 5-13 years of age. Pediatr Infect Dis J 33(11):1128–1133. https://doi.org/10.1097/INF.0000000000000410
Nyandiko WM, Otieno-Nyunya B, Musick B, Bucher-Yiannoutsos S, Akhaabi P, Lane K et al (2010) Outcomes of HIV-exposed children in western Kenya: efficacy of prevention of mother to child transmission in a resource-constrained setting. J Acquir Immune Defic Syndr 54(1):42–50. https://doi.org/10.1097/QAI.0b013e3181d8ad51
Pariente G, Leibson T, Carls A, Adams-Webber T, Ito S, Koren G (2016) Pregnancy-Associated Changes in Pharmacokinetics: A Systematic Review. PLoS Med 13(11):e1002160. https://doi.org/10.1371/journal.pmed.1002160
Poblano A, Figueroa L, Figueroa-Damian R, Schnaas L (2004) Effects of prenatal exposure to Zidovudine and Lamivudine on brainstem auditory evoked potentials in infants from HIV-infected women. Proc West Pharmacol Soc 47:46–49
Prieto LM, Gonzalez-Tome MI, Munoz E, Fernandez-Ibieta M, Soto B, Alvarez A et al (2014) Birth defects in a cohort of infants born to HIV-infected women in Spain, 2000-2009. BMC Infect Dis 14:700. https://doi.org/10.1186/s12879-014-0700-3
Qian X, Jacob F, Song MM, Nguyen HN, Song H, Ming GL (2018) Generation of human brain region-specific organoids using a miniaturized spinning bioreactor. Nat Protoc 13(3):565–580. https://doi.org/10.1038/nprot.2017.152
Qian X, Nguyen HN, Song MM, Hadiono C, Ogden SC, Hammack C et al (2016) Brain-Region-Specific Organoids Using Mini-bioreactors for Modeling ZIKV Exposure. Cell 165(5):1238–1254. https://doi.org/10.1016/j.cell.2016.04.032
Qian X, Song H, Ming GL (2019) Brain organoids: advances, applications and challenges. Development 146(8). https://doi.org/10.1242/dev.166074
Rice ML, Zeldow B, Siberry GK, Purswani M, Malee K, Hoffman HJ et al (2013) Evaluation of risk for late language emergence after in utero antiretroviral drug exposure in HIV-exposed uninfected infants. Pediatr Infect Dis J 32(10):e406–e413. https://doi.org/10.1097/INF.0b013e31829b80ee
Robertson K, Liner J, Meeker RB (2012) Antiretroviral neurotoxicity. J Neurovirol 18(5):388–399. https://doi.org/10.1007/s13365-012-0120-3
Robertson KR, Su Z, Margolis DM, Krambrink A, Havlir DV, Evans S et al (2010) Neurocognitive effects of treatment interruption in stable HIV-positive patients in an observational cohort. Neurology 74(16):1260–1266. https://doi.org/10.1212/WNL.0b013e3181d9ed09
Rondinini C, Venerosi A, Branchi I, Calamandrei G, Alleva E (1999) Long-term effects of prenatal 3'-azido-3'-deoxythymidine (AZT) exposure on intermale aggressive behaviour of mice. Psychopharmacology (Berl) 145(3):317–323
Rubin LH, Maki PM, Springer G, Benning L, Anastos K, Gustafson D et al (2017) Cognitive trajectories over 4 years among HIV-infected women with optimal viral suppression. Neurology 89(15):1594–1603. https://doi.org/10.1212/WNL.0000000000004491
Saitoh A, Hull AD, Franklin P, Spector SA (2005) Myelomeningocele in an infant with intrauterine exposure to efavirenz. J Perinatol 25(8):555–556. https://doi.org/10.1038/sj.jp.7211343
Saylor D, Dickens AM, Sacktor N, Haughey N, Slusher B, Pletnikov M et al (2016) HIV-associated neurocognitive disorder--pathogenesis and prospects for treatment. Nat Rev Neurol 12(4):234–248. https://doi.org/10.1038/nrneurol.2016.27
Schweinsburg BC, Taylor MJ, Alhassoon OM, Gonzalez R, Brown GG, Ellis RJ et al (2005) Brain mitochondrial injury in human immunodeficiency virus-seropositive (HIV+) individuals taking nucleoside reverse transcriptase inhibitors. J Neurovirol 11(4):356–364. https://doi.org/10.1080/13550280591002342
Serghides, L. (2018) Changes in Brain Volume and Cognition in Mice Exposed In Utero to ABC/3TC-ATV/RTV. Paper presented at the Conference on Retroviruses and Opportunistic Infections (CROI), Boston, Massachusetts.
Shallie PD, Naicker T (2019) The placenta as a window to the brain: A review on the role of placental markers in prenatal programming of neurodevelopment. Int J Dev Neurosci 73:41–49. https://doi.org/10.1016/j.ijdevneu.2019.01.003
Shamsuddin H, Raudenbush CL, Sciba BL, Zhou YP, Mast TC, Greaves WL et al (2019) Evaluation of Neural Tube Defects (NTD) After Exposure to Raltegravir During Pregnancy. J Acquir Immune Defic Syndr. https://doi.org/10.1097/QAI.0000000000002031
Sibiude J, Le Chenadec J, Bonnet D, Tubiana R, Faye A, Dollfus C et al (2015) In utero exposure to zidovudine and heart anomalies in the ANRS French perinatal cohort and the nested PRIMEVA randomized trial. Clin Infect Dis 61(2):270–280. https://doi.org/10.1093/cid/civ260
Sibiude J, Mandelbrot L, Blanche S, Le Chenadec J, Boullag-Bonnet N, Faye A et al (2014) Association between prenatal exposure to antiretroviral therapy and birth defects: an analysis of the French perinatal cohort study (ANRS CO1/CO11). PLoS Med 11(4):e1001635. https://doi.org/10.1371/journal.pmed.1001635
Sirois PA, Huo Y, Williams PL, Malee K, Garvie PA, Kammerer B et al (2013) Safety of perinatal exposure to antiretroviral medications: developmental outcomes in infants. Pediatr Infect Dis J 32(6):648–655. https://doi.org/10.1097/INF.0b013e318284129a
Sloan SA, Andersen J, Pasca AM, Birey F, Pasca SP (2018) Generation and assembly of human brain region-specific three-dimensional cultures. Nat Protoc 13(9):2062–2085. https://doi.org/10.1038/s41596-018-0032-7
Sloan SA, Darmanis S, Huber N, Khan TA, Birey F, Caneda C et al (2017) Human Astrocyte Maturation Captured in 3D Cerebral Cortical Spheroids Derived from Pluripotent Stem Cells. Neuron 95(4):779–790 e776. https://doi.org/10.1016/j.neuron.2017.07.035
Slogrove AL, Becquet R, Chadwick EG, Cote HCF, Essajee S, Hazra R et al (2018) Surviving and Thriving-Shifting the Public Health Response to HIV-Exposed Uninfected Children: Report of the 3rd HIV-Exposed Uninfected Child Workshop. Front Pediatr 6:157. https://doi.org/10.3389/fped.2018.00157
Smith ML, Puka K, Sehra R, Read SE, Bitnun A (2017) Longitudinal development of cognitive, visuomotor and adaptive behavior skills in HIV uninfected children, aged 3-5 years of age, exposed pre- and perinatally to anti-retroviral medications. AIDS Care 29(10):1302–1308. https://doi.org/10.1080/09540121.2017.1325436
Smurzynski M, Wu K, Letendre S, Robertson K, Bosch RJ, Clifford DB et al (2011) Effects of central nervous system antiretroviral penetration on cognitive functioning in the ALLRT cohort. AIDS 25(3):357–365. https://doi.org/10.1097/QAD.0b013e32834171f8
Son G, Han J (2018) Roles of mitochondria in neuronal development. BMB Rep 51(11):549–556
Sperling RS, Shapiro DE, McSherry GD, Britto P, Cunningham BE, Culnane M et al (1998) Safety of the maternal-infant zidovudine regimen utilized in the Pediatric AIDS Clinical Trial Group 076 Study. AIDS 12(14):1805–1813
Stern AL, Lee RN, Panvelker N, Li J, Harowitz J, Jordan-Sciutto KL, Akay-Espinoza C (2018) Differential Effects of Antiretroviral Drugs on Neurons In Vitro: Roles for Oxidative Stress and Integrated Stress Response. J Neuroimmune Pharmacol 13(1):64–76. https://doi.org/10.1007/s11481-017-9761-6
Tang H, Hammack C, Ogden SC, Wen Z, Qian X, Li Y et al (2016) Zika Virus Infects Human Cortical Neural Progenitors and Attenuates Their Growth. Cell Stem Cell 18(5):587–590. https://doi.org/10.1016/j.stem.2016.02.016
Tao Y, Zhang SC (2016) Neural Subtype Specification from Human Pluripotent Stem Cells. Cell Stem Cell 19(5):573–586. https://doi.org/10.1016/j.stem.2016.10.015
Tardieu M, Brunelle F, Raybaud C, Ball W, Barret B, Pautard B et al (2005) Cerebral MR imaging in uninfected children born to HIV-seropositive mothers and perinatally exposed to zidovudine. AJNR Am J Neuroradiol 26(4):695–701
Tau GZ, Peterson BS (2010) Normal development of brain circuits. Neuropsychopharmacology 35(1):147–168. https://doi.org/10.1038/npp.2009.115
Teeraananchai S, Kerr SJ, Amin J, Ruxrungtham K, Law MG (2017) Life expectancy of HIV-positive people after starting combination antiretroviral therapy: a meta-analysis. HIV Med 18(4):256–266. https://doi.org/10.1111/hiv.12421
Tierney AL, Nelson CA (2009) Brain Development and the Role of Experience in the Early Years. Zero Three 30(2):9–13
Tovar-y-Romo LB, Bumpus NN, Pomerantz D, Avery LB, Sacktor N, McArthur JC, Haughey NJ (2012) Dendritic spine injury induced by the 8-hydroxy metabolite of efavirenz. J Pharmacol Exp Ther 343(3):696–703. https://doi.org/10.1124/jpet.112.195701
Tovo PA, Chiapello N, Gabiano C, Zeviani M, Spada M (2005) Zidovudine administration during pregnancy and mitochondrial disease in the offspring. Antivir Ther 10(6):697–699
Tran LT, Roos A, Fouche JP, Koen N, Woods RP, Zar HJ et al (2016) White Matter Microstructural Integrity and Neurobehavioral Outcome of HIV-Exposed Uninfected Neonates. Medicine (Baltimore) 95(4):e2577. https://doi.org/10.1097/MD.0000000000002577
UNAIDS. (2018). Global HIV & AIDS Statistics - 2018 Fact Sheet. Retrieved from http://www.unaids.org/en/resources/fact-sheet
Underwood J, Robertson KR, Winston A (2015) Could antiretroviral neurotoxicity play a role in the pathogenesis of cognitive impairment in treated HIV disease? AIDS 29(3):253–261. https://doi.org/10.1097/QAD.0000000000000538
van de Wijer L, Garcia LP, Hanswijk SI, Rando J, Middelman A, Ter Heine R et al (2019) Neurodevelopmental and behavioral consequences of perinatal exposure to the HIV drug efavirenz in a rodent model. Transl Psychiatry 9(1):84. https://doi.org/10.1038/s41398-019-0420-y
Van Dyke RB, Chadwick EG, Hazra R, Williams PL, Seage GR 3rd. (2016) The PHACS SMARTT Study: Assessment of the Safety of In Utero Exposure to Antiretroviral Drugs. Front Immunol 7:199. https://doi.org/10.3389/fimmu.2016.00199
Vannappagari V, Koram N, Albano J, Tilson H, Gee C (2016) Association between in utero zidovudine exposure and nondefect adverse birth outcomes: analysis of prospectively collected data from the Antiretroviral Pregnancy Registry. BJOG 123(6):910–916. https://doi.org/10.1111/1471-0528.13542
Velichkovska M, Surnar B, Nair M, Dhar S, Toborek M (2019) Targeted Mitochondrial COQ10 Delivery Attenuates Antiretroviral-Drug-Induced Senescence of Neural Progenitor Cells. Mol Pharm 16(2):724–736. https://doi.org/10.1021/acs.molpharmaceut.8b01014
Venerosi A, Cirulli F, Capone F, Alleva E (2003) Prolonged perinatal AZT administration and early maternal separation: effects on social and emotional behaviour of periadolescent mice. Pharmacol Biochem Behav 74(3):671–681
Venerosi A, Cirulli F, Lil'p IG, Fiore M, Calamandrei G, Alleva E (2000) Prolonged perinatal exposure to AZT affects aggressive behaviour of adult CD-1 mice. Psychopharmacology (Berl) 150(4):404–411
Venerosi A, Valanzano A, Alleva E, Calamandrei G (2001) Prenatal exposure to anti-HIV drugs: neurobehavioral effects of zidovudine (AZT) + lamivudine (3TC) treatment in mice. Teratology 63(1):26–37. https://doi.org/10.1002/1096-9926(200101)63:1<26::AID-TERA1005>3.0.CO;2-G
Volberding PA, Lagakos SW, Koch MA, Pettinelli C, Myers MW, Booth DK et al (1990) Zidovudine in asymptomatic human immunodeficiency virus infection. A controlled trial in persons with fewer than 500 CD4-positive cells per cubic millimeter. The AIDS Clinical Trials Group of the National Institute of Allergy and Infectious Diseases. N Engl J Med 322(14):941–949. https://doi.org/10.1056/NEJM199004053221401
W.H.O (2018). Mother-to-child transmission of HIV. Retrieved from https://www.who.int/hiv/topics/mtct/about/en/
White AJ (2001) Mitochondrial toxicity and HIV therapy. Sex Transm Infect 77(3):158–173. https://doi.org/10.1136/sti.77.3.158
Whitehead N, Potterton J, Coovadia A (2014) The neurodevelopment of HIV-infected infants on HAART compared to HIV-exposed but uninfected infants. AIDS Care 26(4):497–504. https://doi.org/10.1080/09540121.2013.841828
Williams PL, Crain MJ, Yildirim C, Hazra R, Van Dyke RB, Rich K et al (2015) Congenital anomalies and in utero antiretroviral exposure in human immunodeficiency virus-exposed uninfected infants. JAMA Pediatr 169(1):48–55. https://doi.org/10.1001/jamapediatrics.2014.1889
Williams PL, Marino M, Malee K, Brogly S, Hughes MD, Mofenson LM, Team PC (2010) Neurodevelopment and in utero antiretroviral exposure of HIV-exposed uninfected infants. Pediatrics 125(2):e250–e260. https://doi.org/10.1542/peds.2009-1112
Wise ME, Mistry K, Reid S (2002) Drug points: Neuropsychiatric complications of nevirapine treatment. BMJ 324(7342):879
Xu P, Wang Y, Qin Z, Qiu L, Zhang M, Huang Y, Zheng JC (2017) Combined Medication of Antiretroviral Drugs Tenofovir Disoproxil Fumarate, Emtricitabine, and Raltegravir Reduces Neural Progenitor Cell Proliferation In Vivo and In Vitro. J Neuroimmune Pharmacol 12(4):682–692. https://doi.org/10.1007/s11481-017-9755-4
Yoon KJ, Ringeling FR, Vissers C, Jacob F, Pokrass M, Jimenez-Cyrus D et al (2017a) Temporal Control of Mammalian Cortical Neurogenesis by m(6)A Methylation. Cell 171(4):877–889 e817. https://doi.org/10.1016/j.cell.2017.09.003
Yoon KJ, Song G, Qian X, Pan J, Xu D, Rho HS et al (2017b) Zika-Virus-Encoded NS2A Disrupts Mammalian Cortical Neurogenesis by Degrading Adherens Junction Proteins. Cell Stem Cell 21(3):349–358 e346. https://doi.org/10.1016/j.stem.2017.07.014
Zash R, Makhema J, Shapiro RL (2018) Neural-Tube Defects with Dolutegravir Treatment from the Time of Conception. N Engl J Med 379(10):979–981. https://doi.org/10.1056/NEJMc1807653
Acknowledgments
This work was supported grants from National Institutes of Health (R35NS097370 and U19AI131130 to G-l.M.) and (R21MH118037 to K.M.C.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Schnoll, J.G., Temsamrit, B., Zhang, D. et al. Evaluating Neurodevelopmental Consequences of Perinatal Exposure to Antiretroviral Drugs: Current Challenges and New Approaches. J Neuroimmune Pharmacol 16, 113–129 (2021). https://doi.org/10.1007/s11481-019-09880-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11481-019-09880-z